Industrial Robot’s Joanne Pransky interviews Hugh Herr, head of the Biomechatronics Research Group and Center for Extreme Bionics at MIT.

|
Listen to this article
|
As a teenager, Dr. Hugh Herr was a highly competitive mountain climber, until at the age of 17 he had to have both legs amputated below the knees after suffering severe frostbite during a 1982 mountain expedition. As a result of this experience, he directed his efforts and talent to try to improve the mobility of people with disabilities.
Considered one of the top biomechatronics researchers in the world, Herr heads the Biomechatronics Research Group and the Center for Extreme Bionics at the Massachusetts Institute of Technology (MIT). His research programs seek to advance technologies that promise to accelerate the merging of body and machine, including device architectures that resemble the body’s musculoskeletal design, actuator technologies that behave like muscle, and control methodologies that exploit principles of biological movement.
Herr is also a leading inventor in the field of bionics and biomechanics, producing several groundbreaking products that have already made a significant impact on physically challenged people. To bring his inventions to market, Herr founded a spin-off company out of MIT under the name iWalk in 2007, which was relaunched as BionX Medical Technologies Inc. in 2015, and acquired by Ottobock in 2017.
Herr was recently interviewed by Joanne Pransky for Industrial Robot. That interview is reprinted below, with minor modifications. The original interview can be found here.
Pransky: What commercialized prostheses have you developed?
Figure 1: The Össur Rheo Knee and Rheo Knee XC, transfemoral external knee prostheses that use magnetorheological fluid, were developed by Herr and his MIT Biomechatronics Group.
Herr: At my lab at MIT, thus far there have been two inventions or developments that have been commercialized. The first was the Rheo, a computer-controlled artificial, external knee to be used by persons that are amputated above the knee (Figure 1). It’s now manufactured by an Iceland company called Össur, the second largest prosthetics and orthotics company in the world.
The second product is called the Empower, and it’s the only robotic powered ankle foot prosthesis on the market. We’re working on a third now device, but it’s not quite a product.
Pransky: What are the biggest technical challenges remaining for Empower?
Herr: If, for example, you asked me what the dominant improvement of powered ankles would be in the next 10 to 20 years, I think first it will be the motor technology. Motors are getting better and better. Believe it or not, one would think that everything under the sun has been invented in motor technology, but it’s not true. So, I expect tremendous innovation in motor topology.
The second is linking a wearable robot to the nervous system, implantable sensors that can extract motor intent from the human and also, techniques for reflecting sensory information from the prosthesis into the nervous system. A person can feel the position of the limb or feel a surface, like a skin sensation.
We’ll see some improvements with batteries, but I think they’ll be small compared to those first two developments. Battery technology may get around 50% better, but it won’t be an order of magnitude.
All this adds up to a future limb that is smaller, lighter, quieter and directly embodied into the nervous system, where the human wearing it feels whole, feels complete and feels like their limb has been manifested again after an amputation.
Pransky: How many Empowers been sold to date, and what percentage is in the U.S.?
Herr: I think it is now about 2,000. The U.S. represents about 50% of the world market for prosthetics and orthotics.
Pransky: In the U.S., is the Empower typically covered by the federal Centers for Medicare & Medicaid Services (CMS), or private insurers, or veterans that qualify?
If you asked me what the dominant improvement of powered ankles would be in the next 10 to 20 years, I think first it will be the motor technology. Motors are getting better and better. Believe it or not, one would think that everything under the sun has been invented in motor technology, but it’s not true.
Herr: A standard prosthesis that’s been on the market for some time would be typically recognized by CMS. There would be a reimbursement code and a reimbursement price, and then a coverage decision by CMS. It’s a three-legged stool in order to have CMS and private insurance cover a prosthesis. With new technology, it takes a very long time to get to that reimbursement stage.
Currently, the Empower, which costs about $40,000–$50,000 including clinical servicing, has a CMS reimbursement code, but there’s no price on that code nor is there a suggested reimbursement. Because CMS doesn’t recognize the technology, private insurances don’t either.
The only reimbursement for the Empower today is through the Department of Defense. For example, a soldier who has recently lost a limb on the war field can get the Empower. The Veteran’s Administration (VA) has been fantastic. They reimburse the Empower as does the U.S. Department of Labor’s Office of Workers’ Compensation Programs (OWCP).
When you add those three up, it’s about 14% of the U.S. market. Most people, unfortunately, are not able to get the Empower because of the lack of reimbursement.

Figure 2: The Empower, now in its third generation and distributed by Ottobock, was originally designed by Herr and is the only lower leg prosthetic with an active ankle joint.
Pransky: What motivated you to sell your company, BionX Medical Technologies to Ottobock in 2017?
Herr: Ottobock is the largest prosthetics and orthotics company in the world, headquartered in Germany. They’re a fantastic company with excellent engineering; they’re very thoughtful and thorough in their product development. Because of that, they have a whole host of remarkable products, and I couldn’t think of a better company to take over and be the stewards of the powered foot ankle technology that we developed.
Pransky: How did you manage both your roles at MIT and the startups you co-founded? Did you ever think of leaving your teaching position to work full time for iWalk or BionX?
Herr: Not seriously. I did ask the question, but I never made a clear decision in that direction. iWalk – and what later led to BionX – has struggled with reimbursement, but technologically we’ve always had a strong team.
Pransky: What is the greatest business lesson you’ve learned?
Herr: For wearable robotics in the medical domain, not in the non-medical commercial domain, the greatest hurdle to global translation is reimbursement. In no way is it U.S. Food and Drug Administration (FDA) regulatory approvals.
The FDA is fairly straightforward – if you do cross your T’s and dot your I’s, you will get the device approved in time, but reimbursement is very, very challenging. Either you’re a very large company that has many, many products and you can spend a decade working on reimbursement for a new innovation, or you are small and you maybe develop a device that already has reimbursement, but you expand the device’s clinical efficacy.
Or you have endless money, you are a billionaire, and you can spend 10 years working on reimbursement. That’s the key challenge: It’s very difficult for a small startup to weather the storm of reimbursement, which, unfortunately, often takes a decade or so.
Pransky: Is it the same outside of the U.S.? Is reimbursement easier, say, in Asia or Europe, for example?
For wearable robotics in the medical domain… the greatest hurdle to global translation is reimbursement.
Herr: Every country is different. For some countries, such as Norway, a very small but oil rich and liberal country, reimbursement is very simple. In Germany, if a person needs a novel prosthesis and is denied, I think they can actually sue and that triggers a change in policy and a pathway towards reimbursement. Every system has its own levers.
Pransky: Is there the prospect – and maybe this is the third product that you’re developing – of a neural interface?
Herr: Basically, the top three objectives of my MIT research group are first, to link wearable machines bidirectionally and with high fidelity, to the peripheral nervous system or to muscles and nerves to both sense motor intent from the central nervous system, as well as to reflect sensory information from the worn mechatronic device onto the nervous system for afferent sensations.
The second is to understand how robots and machines can be attached to the body mechanically in a safe, comfortable manner.
And the third is how one can build robots that reflect the dynamics, mass and volume of a biological limb.
Pransky: What are some of the required processes to commercialize your groundbreaking neural interface?

Figure 3: The Ottobock Empower
Herr: We have a somewhat unusual approach to neural interfacing. Typically in the field, the neural interface designer assumes that the biological body is fixed and invariant and doesn’t try to restructure the biology in a manner that makes neural communication more tractable.
Often, researchers design synthetics to an existing body that’s deemed invariant and unchanging. We relax that constraint, and we ask the question, how can we redesign the human body, along with synthetics, to enhance neural communication between the brain and a wearable device?
My group has a series of inventions on how to amputate limbs to create a tissue environment that’s more conducive to neural sensing and neurofeedback. We invented a new amputation paradigm.
Pransky: How do you communicate your new amputation paradigm to surgeons worldwide performing the amputation?
Herr: Typically, the invention and scientific preclinical investigations are advanced by my group at MIT. We started with one surgeon on the staff and now we have about three. When there’s sufficient preclinical work or significant scientific basis for the approach and validation, we then proceed towards a first human surgery.
MIT does not do surgeries because MIT is not a hospital, so we’ve collaborated closely with Brigham Women’s Hospital (BWH). We work with plastic surgeon Dr. Matthew Carty who actually does the novel amputation techniques on human patients.
As of April 2020, BWH has performed approximately 23 human-limb amputations. It’s exciting because thus far the procedures have been largely reimbursed by insurance so there’s a clear pathway for global translation of the techniques.
The soft tissue work is one piece of the puzzle. The second is, once you’ve created these tissue interfaces, how can we sense the state of the tissues and recommunicate that to a computer on the external robotic appendage?
For this second piece, our strategy is to implant small magnetic spheres – a BB-like ball with a diameter of about 3 mm that is coated in a biocompatible material such as perylene or titanium. We then inject the beads into any tissue and for our first application we are targeting muscle.
Then with electronic sensors on the surface of the skin, we then measure the magnitudes and orientations of the magnetic field lines created by the implanted spheres. We do an inverse calculation and say, “Where does the sphere have to be in space in order to produce that field?”
As the person moves their phantom wrist, hand and fingers, we will measure very precisely all that movement and communicate each muscle’s length and speed data to the robotic hand and wrist in a master–slave control.
We can then very precisely determine the location of each sphere, even though there are no wires going from the sphere to the electronics. We can mathematically determine their location as the muscle contracts and as it stretches so that we have a precise measurement of muscle length and speed versus time.
We then plan to communicate that state information directly to small computers on a bionic limb, giving the person exquisite control over their bionic limb. This work is now in a preclinical phase; we have not yet implanted humans, but we’re moving very rapidly in that direction.
I describe this as a minimally invasive strategy. It’s invasive because we’re implanting something in the body, but what we’re implanting is passive; with no wires, no electronics required inside the body. Any nurse can implant the beads within tissue and the regulatory hurdle, the cost, will indeed be modest.
Following implantation, one can then apply a master-slave control. Imagine a person who is amputated below the elbow and the person’s forearm muscles are linked in agonist and antagonist pairs forming agonist–antagonist myoneural interfaces – AMIs (Figure 4). We then will implant two magnetic spheres within each muscle. We then will place on just the skin an electronic board the size of a credit card that will measure the length and speed of each muscle.
Thus, as the person moves their phantom wrist, hand and fingers, we will measure very precisely all that movement and communicate each muscle’s length and speed data to the robotic hand and wrist in a master–slave control. This approach will go from the linear space of the muscles directly to the rotary space of the robotic hand.
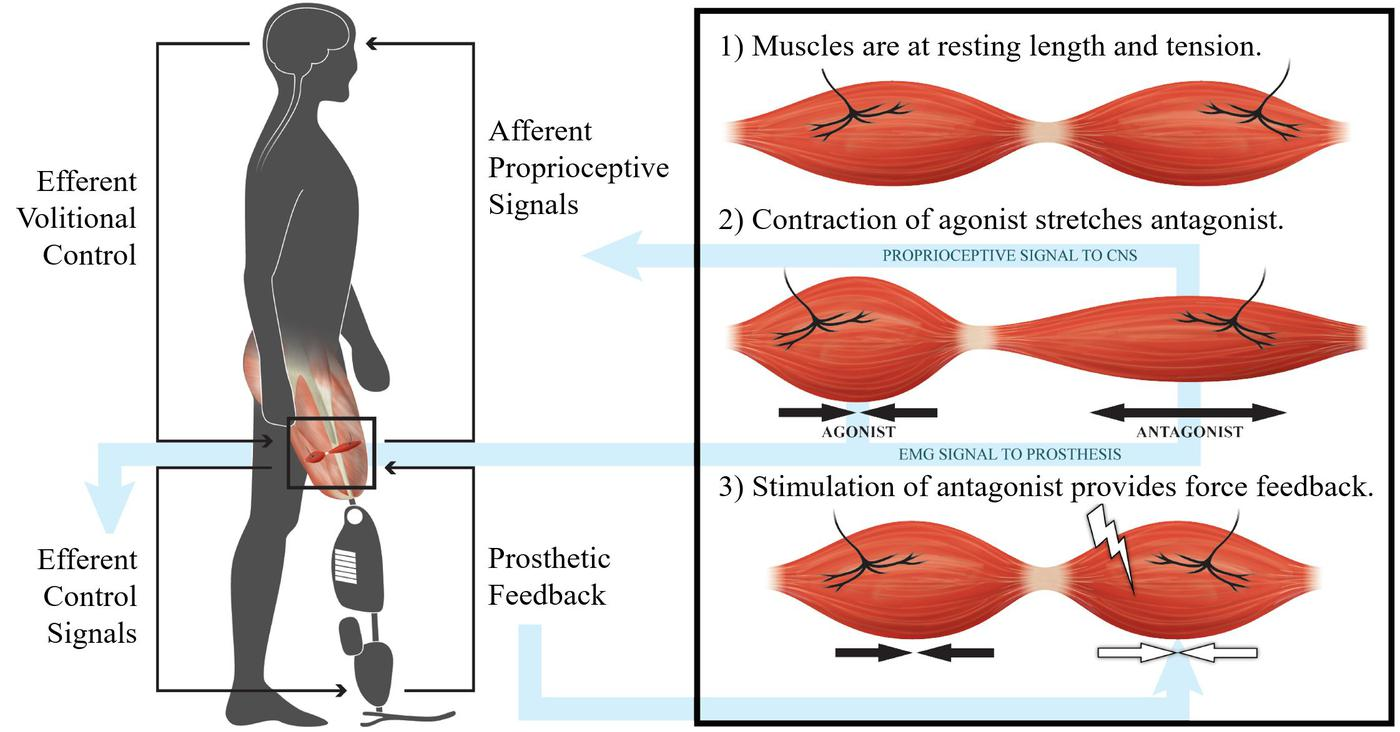
Figure 4: Hugh Herr and the Center for Extreme Bionics at the MIT Media Lab invented the agonist-antagonist myoneural interface (AMI), a method to restore proprioception to persons with amputation Credit: Srinivasan et al., Science Robotics (2017), original artwork by Stephanie Ku
Pransky: Are you also working to develop those hands, elbows or arms as well?
Herr: In the past, my lab focused entirely on dynamic interface. It’s still a focus, but we’re also conducting important research in the areas of neural interfacing and mechanical interfacing as well.
Pransky: What about those who have neural impairment?
Herr: Paralysis caused by spinal cord injury is an area in which we want to make rapid progress. We are interested in central nervous system injury, most specifically spinal cord.
We’re asking the question now, how can small computers, simulators and feedback loops take over the control of biological muscle and restore movement in a person with biological limbs, but limbs that are not connected robustly to the central nervous system?
There’s been a few of those days in my career where not only does everything go right, there’s something that’s truly surprising and remarkable that unfolds before one’s eyes.
Joanne Pransky: What is the proudest moment of your career?
Hugh Herr: I’ve had a few, but they all can be characterized in the same way. For those folks doing science and engineering, it often seems painfully slow. One needs patience that extends out to infinity.
But on occasion, one comes to their lab or startup company and witnesses magic. There’s been a few of those days in my career where not only does everything go right, there’s also something that’s truly surprising and remarkable that unfolds before one’s eyes.
In recent times, such a surprising moment unfolded with our first patient that received the AMI amputation, Jim Ewing, a friend of mine. He damaged his leg after a rock-climbing fall and after years of rehabilitation his leg needed to be amputated. After he received the AMI amputation, he healed. He went through physical therapy.
Ewing came into the MIT Lab, and we strapped the robot to him with all the electrodes measuring the signals from his AMI ankle and subtalar musculature.
Eventually, after sitting and learning how to move the robot by signaling his nerves in his muscles, he stood up and started walking up and down stairs and other terrain. Before our very eyes, through the robot, we witnessed natural movements, natural biomechanics mediated through the mechatronics.
We asked Jim, “Are you trying to move the robot?” He said no… the movements were completely involuntary. He just simply walked down steps and these elaborate motor patterns were communicated through the robot.

Hugh Herr. Source: TED Talk
That was a remarkable day where we witnessed the fact that if you give the brain sensory information from the wearable robot, the brain knows exactly how to control the robot. The robot does not even need a control system.
In fact, biological reflexes and natural biomechanical behaviors can be mediated through the synthetic design, as if it’s a biological appendage.
Pransky: What do you think Ph.D. and masters of engineering students should be doing while in school to best prepare them for the commercial side of robotics?
Herr: It’s always helpful to be a generalist. If one’s knowledge is extremely narrow, it is more difficult to connect the dots in invention and innovation.
Persons that know mechatronic design, control and neural interfacing and those who can connect the dots between all these domains are those people that often invent and innovate. The deep specialist can’t see outside of their dug trench. Many inventions and innovations today happen at the interfaces between formal disciplines, not within formal disciplines.
Pransky: What will your TED Talk be 20 years from now?
Herr: In my second TED Talk, I spoke about neurological embodiment and I had the animation of Birdman, Leonardo da Vinci’s vision of a human with wings. I am very fascinated by the idea that in the future, human designers can design the body itself and redefine who we are. In 100 years, humans as we are today will be unrecognizable. We will collapse our very narrow views of what a human being is; what beauty is; what intelligence is. To me, that’s very, very exciting and I would like to witness such body alchemy in the next 20 years.
 Joanne Pransky was an associate editor for Industrial Robot Journal since 1995. She was also one of the co-founders and the director of marketing of the world’s first medical robotics journal, The International Journal of Medical Robotics and Computer Assisted Surgery.
Joanne Pransky was an associate editor for Industrial Robot Journal since 1995. She was also one of the co-founders and the director of marketing of the world’s first medical robotics journal, The International Journal of Medical Robotics and Computer Assisted Surgery.
Pransky also served as the senior sales and marketing executive for Sankyo Robotics, a manufacturer of industrial robot systems. She consulted for some of the industry’s top robotic and entertainment organizations, including Robotic Industries Association, Motoman, Stäubli, KUKA Robotics, ST Robotics, DreamWorks, Warner Bros., and for Summit Entertainment’s film Ender’s Game, in which she brought never-seen-before medical robots to the big screen.





